Transforming the Trauma Centre to Tackle COVID-19
Since April 3rd, the Montreal General Hospital has been one of the designated centres for patients with COVID-19. Despite this new mission, the MGH must maintain the regular activities of its Trauma Centre, one of only three centres in the province with the proper expertise to treat adults presenting with acute physical trauma.
The COVID-19 pandemic is changing the look – and the treatment processes – of the Montreal General Hospital’s Dr. David S. Mulder Trauma Centre. “We often have multiple casualties coming into the Trauma Centre,” says Dr. Kosar Khwaja, Trauma Surgeon and Critical Care Physician at the McGill University Health Centre. “But now, with the COVID-19 pandemic, we are trying to isolate each patient to minimize infection risks.” But if more than one patient requires treatment in the trauma bay, the choice is either slowing treatment by limiting the space to one patient at a time, or risk having one patient infecting the other; further, sterilizing the room after the patient leaves can take up to 30 minutes.
In all, keeping the COVID-19 virus from infecting anyone in the trauma bay had become a space-and-time-consuming operation.
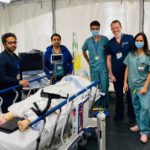
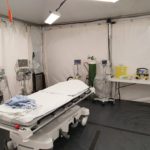
So Dr. Khwaja proposed a solution that is both simple and innovative: a fully equipped Resuscitation Tent erected in the parking lot, directly outside the trauma bay, to enable the trauma team to treat more than one patient in isolation.
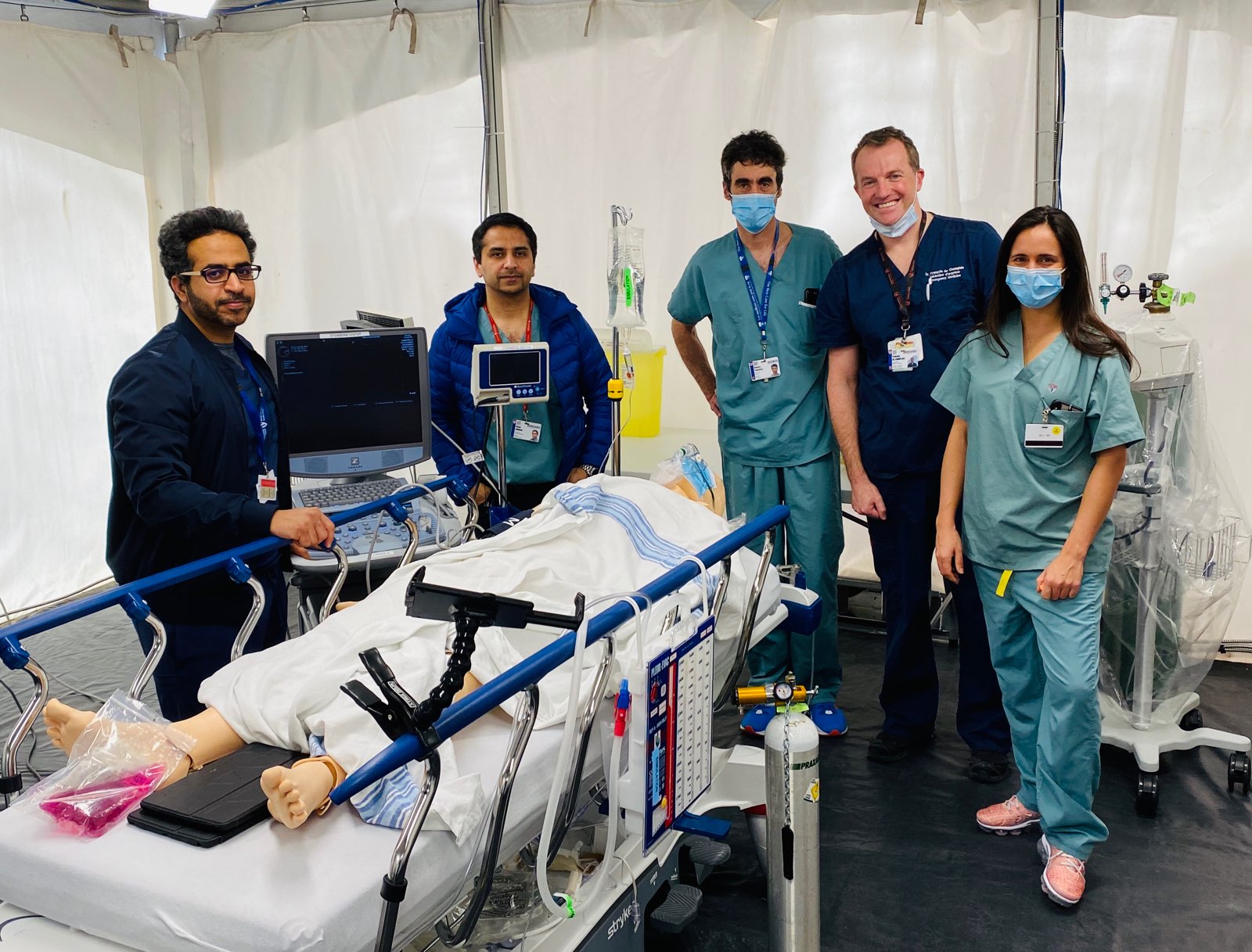
The tent opened for patients on Wednesday April 15th and immediately proved its worth. “It’s given us more area to work in the emergency department, essentially extending the department by adding a new fully functional room where we can resuscitate any critical patient that comes to us,” says Dr. Khwaja. “It has been well received by the emergency team and the trauma surgery group. And we can use it not only for trauma patients, but for any critically ill patient.” While currently set up for one patient, the tent was designed so that, if required, it could hold up to three patients.
Astonishingly, the entire process of getting the facility in place – from proposal to accepting patients – took less than a week. “Everyone was supportive, from the administration to the people working the front lines. Within 48 hours of drafting a proposal, we had received a positive response from administration. Everybody stepped up quickly and rallied around the project, and we got the tent up in record time.” Trauma surgeons, anesthesiologists, ED physicians and nurses were consulted to ensure the proper equipment was in place, and that patient flow was optimized. The team received input from infection control and biomedicine specialists.
The technical services team built and outfitted the structure within three days, including heating to withstand the cold Montreal spring and a ventilation system to ensure healthy air circulation, while the multimedia team set up cameras. Prior to opening the Resuscitation Tent, the team conducted several simulations to ensure the safety of patients and healthcare workers. “Everybody went the extra mile to get this off the ground. It was a collaborative effort, with everybody doing what they needed to do very efficiently.”
The rapid set-up can be ascribed, at least in part, to the depth of experience at the Montreal General Hospital. Dr. Khwaja has worked with the International Committee of the Red Cross (ICRC) and the Canadian Red Cross in similar facilities around the world and was the Canadian Public Health Agency lead for Disaster Preparedness for the 2010 Winter Olympics at Whistler, BC. Several other trauma team members involved with the MUHC’s Global Surgery Program have also worked with international organizations in field hospitals. “We are fortunate to be able to draw on the expertise we have right here at the hospital,” he says.
The Montreal General’s Resuscitation Tent had also attracted the attention from the Lachine General Hospital, and has been a model for them as they set up their own emergency department tents.
While the trauma patient profile has shifted somewhat due to the COVID-19 pandemic lockdown, Dr. Khwaja notes, “With fewer cars on the road, we have had less car crash victims, but, people are still falling and sustaining injuries in their homes. At some point, though, people will start returning to work and school, and we will see more of the types of trauma we typically receive this time of the year, like car and motocycle crashes and bicycle related injuries.. Yet COVID-19 will persist past the first wave of the pandemic, and we will still have to take the infectious precautions for our patients,” he says. “So our Resuscitation Tent will help us treat patients not just for the next couple of weeks, but throughout the coming months.”